Medical Technology Brings Advancement and Questions
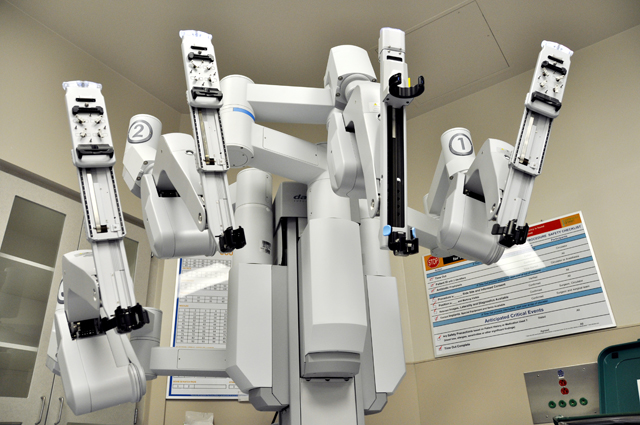
The four arms of the da Vinci surgical system are controlled by a doctor at a remote station and operate inside the human body. The da Vinci system and other high-tech innovations are revolutionizing how doctors learn and practice medicine. Photo by David Barer.
By David Barer
For Reporting Texas
AUSTIN — Leonardo da Vinci toiled over human and animal bodies 700 years ago, slowly dissecting and analyzing them, with now-antiquated methods he pioneered to advance medical understanding. Today, Leonardo’s name is synonymous with a cutting-edge technology, the da Vinci robotic surgery system, that is fast-forwarding surgical procedures and how young doctors learn about medicine.
It’s a robotic arm that can reduce an aging doctor’s tremors during surgery. It’s a three-dimensional, interactive visualization of a human kidney allowing students to examine the organ’s underside before removing it from a cadaver. It’s a surgical simulation a gynecologist can use to rehearse a hysterectomy technique hundreds of times sans patients.
For all of the benefits, however, such innovations could create new problems: a division between those who can afford the technology and those who can’t, as well as the loss of traditional surgery skills. In addition, doctors are quick to point out that while robotics may be the future, and simulated surgery training for robotics will be more prevalent, the nuances of operating on real people and dissecting actual cadavers aren’t easily replicated.
With high technology “entering into the surgical sciences, you can expect paradigm shifts, or leaps forward,” said Dr. Thomas Payne, an obstetrician gynecologist and medical director at the Texas Institute for Robotic Surgery at St. David’s North Austin Medical Center. Payne also speaks for Intuitive Surgical, the makers of the da Vinci robotic surgery system and the simulators used to train the physicians that use it.
At the forefront of these surgical technologies is the da Vinci robot, a remote-controlled device that allows a doctor to peer inside a patient’s body at 15-times magnification and conduct procedures with joysticks and three machine arms equipped with pincers, scissors, grips, cauterizers and other specialized tools.
The robot could be mistaken for a science fiction torture device, but it might be the best reducer of post-operation pain since Demerol.
In a laparotomy, now considered the traditional method of surgery, surgeons cut a large incision into the abdomen and pull the skin apart to expose the patients’ internal organs. Laparoscopic surgery is the practice of introducing the instruments and a camera into the body through small holes and performing the surgery completely using a display screen. Still, a standard laparotomy procedure could leave a patient in the hospital for several days on narcotics.
The da Vinci is laparoscopy 2.0.
“The amazing thing is that the patients don’t have pain,” said Bill Rowe, an obstetrician and gynecological surgeon at The Woman’s Hospital of Texas in Houston. “Now, under the robot, many times we can send the patient home the same day … at the most the next day, and there is essentially no pain.”
The robot’s precision and how it couples with the body through four finger-sized holes amounts to minimal cutting of the skin, nerve and soft-tissue damage and inflammation – the major causes of post-op pain.
The patient’s comfort comes at steep price for medical practices and hospitals. A single robot costs about $1.5 million. In addition, the maintenance contract for the machine runs about $500,000 for three years. The instruments at the end of the robot’s arms must also be changed after 20 uses, at a cost of $1,000 per instrument. All told, it’s an investment of nearly $3 million per machine.
The big price tag means most hospitals using the da Vinci are large facilities with deep pockets.
On the other hand, you can’t put a value on the life of a patient Rowe said. While the machine creates an artificial environment for the surgeon where movement and vision are enhanced far beyond human capability. Rowe, who says he has no financial interest in da Vinci, looks forward to other companies entering the market to help reduce costs.
“Even for already seasoned doctors … the more you do the robot surgery, the more you lose your old ways to do it without the robot, so that is one of the major disadvantages,” Rowe said. In every procedure there could be complications requiring the doctor to revert to a laparotomy-style operation. A doctor who rarely performs surgery without the robot’s precision and magnified, three-dimensional optics could be stymied by such a complication.
Dr. Michael Breen, an obstetrician gynecologist and director of robotics and minimally invasive surgery at the University of Texas Southwest OB-GYN residency program in Austin, believes the advantages of using robotic technology go to the patient. Going through medical school 31 years ago and watching the profession change Breen has learned that, in medicine, old habits don’t die hard.
Breen says he was intimidated at first sight by the robot-machine but found that after a couple dozen procedures he could perform surgery with more precision than ever before.
“It’s like having Mini-Me dropped inside someone during surgery,” he said. “It’s just a tremendous perspective. I can perform a hysterectomy using both laparoscopic and the da Vinci, so I can choose which one I would use, and I choose to use the da Vinci.
“There certainly are some old techniques that have gone by the wayside,” Breen said. But “all the benefits … for the patient are much more important than being able to say, ‘Well, this is a traditional technique that doctors used for years.’”
Some medical practices cannot be easily replicated by machine or technology, insists Dr. Omid Rahimi, an assistant professor at the University of Texas Health Science Center in San Antonio and director of the human anatomy program there, who oversees the receipt and dissection of cadavers.
A few modern conveniences notwithstanding, Rahimi teaches his students about anatomy the same way that da Vinci learned more than 700 years ago — by dissection. The willed-body program receives between 100 and 150 cadavers each year. Each body is dissected from head to toe over the course of a year or more by Rahimi and his students in the health science center’s basement laboratory.
Yet even in this most time-honored of medical traditions, technological advances are creeping in. Rahimi himself is developing an iPad app that will show snapshots of minute portions of human organs and anatomy to aid students in learning their lessons.
Perhaps the biggest advance of all is the addition of three-dimensional, digital representations of human bodies allowing students to visualize organs and body parts intensively without ever making an incision in a cadaver.
Rahimi sees three-dimensional representations as an excellent enhancement to his student’s learning but doesn’t think digital dissection will ever completely replace the cadaver. Dead bodies prepare a student for the stark realities of the medical profession.
“[Students] have to very quickly come to grips with ideas such as death, dying and, ‘I’m going to work on this cadaver that used to be someone’s lover, a real person, a dynamic, vibrant person,’” Rahimi said. “There is no way that you can convey that, ever, from a computer software or 3-D experience.”
For now, technology appears poised to alter the practice of medicine at an ever-faster clip by augmenting decidedly human skills, not replacing them. According to Breen, a surgeon’s knowledge is tantamount to the instruments he uses.
“The da Vinci won’t do any operation on anyone. It only does what the surgeon does. It’s a mirror of the surgeon’s hands,” Breen said. “The easy part of surgery is the actual scalpel motion. The hard part is knowing when to use it and what it is you’re trying to do with it.”